It is new, but not entirely. The coronavirus upending the world right now is so similar to the severe acute respiratory syndrome (SARS) virus of 2002–03 that virologists opted to simply call it SARS-CoV-2.
Yet there seem to be some crucial differences between the virus that caused an epidemic 17 years ago and the one causing a global pandemic today. The good news is that relative to the number of infections, the virus does not seem to be quite as deadly as the earlier SARS virus was. SARS-CoV-1 infected around 8,000 people and killed roughly 1 in 7, whereas the estimated death rate for known cases of SARS-CoV-2 — while still uncertain — is much lower, perhaps even less than 1 in 70.
The bad news is that SARS-CoV-2 already has spread far more widely that SARS-CoV-1 did, in part because of the milder symptoms that many people experience and the virus’s longer incubation period — the time between being infected and showing symptoms of illness. Those things mean that infected people are more likely to unwittingly spread SARS-CoV-2 than they were with SARS-CoV-1.
To understand the reasons for these differences, researchers are intensively studying the three-dimensional structure of the viral proteins and, in particular, the ones it uses to infect human cells and reproduce inside them. Such knowledge might offer vital clues for developing therapies and a vaccine — some of which are already being tested.
Eye-catching spikes
Knowledge about the new virus has advanced rapidly. The part that has received most attention so far is the spike protein: the one that sticks out in electron microscope images. Studded with these proteins, the virus looks somewhat like a crown (“corona” is Latin for crown).
Scientists focused their attention on the spike because they know it plays a crucial role in infection, performing not one but several key functions for the virus: allowing it to recognize, bind to and enter host cells.
CREDIT: NIH
The first genetic sequence of the virus was made available to researchers on January 11. Less than six weeks later, on February 19, researchers from the lab of structural biologist Jason McLellan at the University of Texas at Austin published a paper in Science revealing the three-dimensional structure of SARS-CoV-2’s spike protein. “It looks like a mushroom, with a head and a stem,” says Nianshuang Wang, one of the researchers in McLellan’s lab who worked around the clock to derive the structure.
The head of the spike, also known as S1, is the part that first attaches to a host cell. More specifically, it binds to a receptor called ACE2 that sits on the outside surface of the cells in some of our tissues, including those lining the inside of the lungs. The normal function of ACE2 is not, of course, to help viruses get in — it plays a role in blood-pressure regulation, among other things. But both SARS-CoV-2 and the earlier, closely related SARS-CoV-1 have co-opted ACE2 for their own purposes.
In both viruses, the S1 spike head uses a string of amino acids called the receptor binding motif to recognize the ACE2 receptor and latch onto it. But the structure of this motif is surprisingly different in SARS-CoV-1 and SARS-CoV-2, Wang says. Whereas overall the amino acid sequences that make up the spike protein are about 80 percent identical between the two viruses, their receptor binding motifs are only around 50 percent the same.
Because of its crucial role in recognizing ACE2, the binding motif’s sequence and structure can have a major effect on the likelihood that the spike protein will bind to the receptor, as reflected by a measure called binding affinity. An experiment reported in the same Science paper showed that the SARS-CoV-2 spike protein’s binding affinity to ACE2 is 10 to 20 times higher than that of the SARS-CoV-1 spike protein. This might explain why SARS-CoV-2 is more easily transmitted from one person to another than SARS-CoV-1 ever was, Wang says. “But we need more hard evidence to confirm this.”
Because the structure of ACE2 receptors differs from one species to another, the virus would had to have made quite a few changes to gain the ability to infect people, says virologist Ding Xiang Liu of the South China Agricultural University in Guangzhou, who coauthored a 2019 overview in the Annual Review of Microbiology on how human coronaviruses interact with their hosts.
Animal markets where many different species are brought into close proximity are ideal environments for viruses to experiment with this. “Therefore, we should avoid human activities that encourage these events, such as the consumption of wild animals,” Liu says.
Forced fusion
After the spike protein attaches to an ACE2 receptor, scientists believe that the membrane surrounding the cell may then engulf the virus to bring it inside and transport it to a lysosome. This is a bubble containing enzymes that, as part of an evolved defense mechanism, cut the proteins of potential intruders into harmless little bits.
But the spike proteins of viruses such as SARS-CoV-1 and SARS-CoV-2 have, in turn, evolved to take advantage of the cell’s attempt to defend itself. In fact, it is only after one or more of the cell’s enzymes have cut into it that the protein is able to take the next step: dragging the membranes surrounding the virus and lysosome closer until they fuse. This allows the virus’s genetic material to escape from the lysosome into the cell.
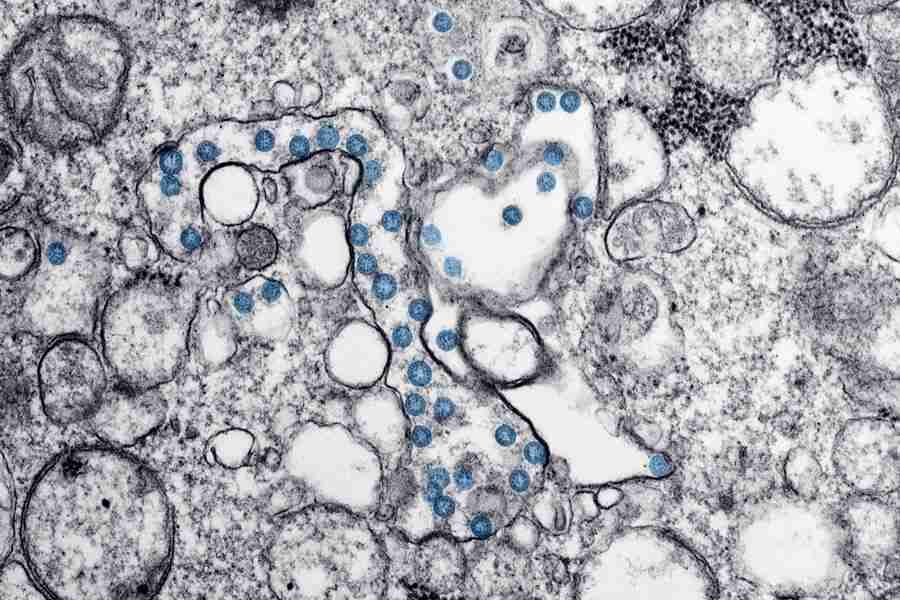
This transmission electron microscope image is of an isolate from a US Covid-19 patient. Particles of SARS-CoV-2, the virus that causes the disease, are colorized blue.
CREDIT: CDC / HANNAH A BULLOCK; AZAIBI TAMIN
The genetic material of these viruses is RNA, not DNA. RNA is the same molecule that our cells use to relay genetic instructions from the nucleus out to the location where proteins are built. So when the viral RNA is released from the lysosome, the cells quickly get to work building the proteins it prescribes, allowing the virus to reproduce and expand.
This is when things can get dangerous, Liu says. Although we think of the immune system as a lifesaver — and generally, it is — in some patients a massive production of viral RNA and proteins can cause the immune system to go into overdrive, leading to severe illness, even death. Such an “exuberant” immune response is the “main cause of tissue damage and organ failure” that is observed in many of the patients who die from the virus-caused illness Covid-19, Liu says.
Viral vaccines
Several trials are testing various existing drugs that were developed to treat other diseases, including some viral infections, to try to suppress SARS-CoV-2 (for example, by interfering with its replication). But the most promising route, many scientists believe, is to develop a vaccine that will help our immune systems do a better job at fighting off SARS-CoV-2 infections to begin with.
Teams are racing to develop such vaccines, which may include dead or weakened viruses or, more commonly, just a few specific fragments of them, paired with a few other substances that stimulate the immune system to get to work. The body responds by making antibodies that will attach to any molecules resembling the contents of the vaccine, tagging the virus for destruction by white blood cells.
But vaccines could sabotage SARS-CoV-2 in other ways, too. For example, antibodies that attach to the receptor binding motif of the spike protein might stop it from binding to the ACE2 receptor. And that would stop the virus from infecting the cell. Antibodies that bind to another part of the spike protein could stop the virus from fusing membranes together and getting its genetic material to the cell’s protein-building facility. Just getting an antibody to bind to the spike protein may not be sufficient, however. Some antibodies won’t affect the protein’s function at all, while others might even enhance it.
The large-scale production of a vaccine containing sufficient amounts of a protein such as SARS-CoV-2 spike protein will likely be difficult and expensive, Wang says: “Proteins are hard to make, and hard to maintain at high quality.” For this reason, some companies are now following a different approach, perhaps inspired by the virus itself. Instead of using the protein, they are using the RNA that contains the instructions to build the protein. Once a person’s cells have built the protein, the immune system can make antibodies in response. Scientists are currently testing a vaccine of this kind containing RNA that codes for the SARS-CoV-2 spike protein.
Wang hopes that new knowledge about the structure of the spike protein will permit a more targeted approach. One could create a vaccine that contains exactly the part of the spike protein the researchers would like the antibody to bind to, or the RNA instructions allowing the cell to build that part by itself, in order to obstruct the virus as much as possible.
Antibody bonanza
About 35 companies and academic institutions are working on a vaccine. But success will take time, and a vaccine is of no help to people who are already infected.
So in addition to trying existing therapies, some researchers are trying to make antibodies to the spike protein in the lab that could be infused into people as drugs. This can be done in a number of ways, for example by injecting the viral spike protein into mice that have been genetically modified to produce antibodies more similar to ours. Tests can then show if any antibodies are effective at blocking the virus.
In a paper published online on March 12 that has yet to be peer-reviewed, a team of researchers in the Netherlands led by molecular biologist Frank Grosveld and virologist Berend-Jan Bosch announced that one of 51 antibodies created with this approach looks especially promising. The team’s experiments show that this antibody, 47D11, can bind to the spike protein of both SARS-CoV-1 and SARS-CoV-2, and can prevent another virus endowed with a SARS-CoV spike protein from infecting cells. (Exactly how the antibody does so is as yet unclear. Even though it attaches to the spike protein’s receptor binding domain, it does not seem to stop the spike protein from binding to the ACE2 receptor.)
The antibody will now be tested to see whether it can prevent infection in mice or other animal models. If those experiments are successful, its safety and effectiveness will then have to be tested in the clinic. In the meantime, however, it may aid in the development of more effective tests for the virus.
“It’s too early to say whether the antibody could serve as an effective therapeutic,” says Wang. “But clearly, it’s a promising first step.”
Eventually, these findings might also inspire a new vaccine containing the part of the protein the 47D11 antibody binds to, or the genetic instructions for our cells to make their own. Vaccines are generally more sustainable, says Wang: Therapeutic antibodies infused into people need to be regularly replenished. But a good vaccine can teach the body, once and for all, to make its own antibodies whenever they are needed — and possibly all in one shot.
10.1146/knowable-031920-1

